Are You at Risk of Heart Disease? Here’s Why You Need a Heart Health Check
Cardiovascular disease is one of the leading causes of death in Australia, accounting for around 24% of all deaths. Many people feel healthy even when heart disease risk is developing silently. A heart health check helps detect early warning signs before serious complications like heart attack or stroke occur.
February is Heart Health Month — a great reminder to understand your heart risk, know your heart numbers, and take proactive steps to protect your cardiovascular health through early screening and prevention.
This guide will help you discover who needs a heart check, the key risk factors tested, what your results mean, and the most effective strategies to lower your risk.
So, keep reading… because prevention is always better than treatment.
What Is a Heart Health Check?
A heart health check is a structured, GP-led cardiovascular risk assessment designed to detect early signs of heart disease before symptoms appear. It measures key health metrics, including blood pressure, cholesterol levels, blood sugar, weight, and lifestyle risk factors, to estimate your likelihood of developing heart disease or stroke over the next 5–10 years.
Let’s explore what a GP actually measures during heart check-up?
What Happens in a Heart Health Check?

During your heart health check, your GP will:
Review Your Medical & Lifestyle History
You’ll be asked about:
- Age and family history of heart disease
- Smoking status
- Diet and physical activity
- Alcohol intake
- Mental health and stress levels
- Existing heart conditions or diabetes
These factors help calculate your overall cardiovascular risk.
Perform Physical Measurements
Your doctor or nurse will measure the key risk factors that contribute to heart disease risk:
- Blood pressure checks—High blood pressure is one of the strongest predictors of heart disease.
- Cholesterol testing—A blood test to assess total cholesterol, LDL (“bad”), HDL (“good”), and triglycerides.
- Blood sugar levels—Elevated glucose can indicate diabetes or pre-diabetes.
- Weight, height, and waist circumference (to assess BMI and abdominal risk).
Calculate Your Cardiovascular Risk
Your GP may use the Australian cardiovascular disease risk calculator (AusCVD) to estimate your risk of experiencing a heart attack or stroke within the next 5–10 years. This personalized assessment helps determine whether lifestyle changes alone are appropriate or whether medication or further investigations are recommended.
The three most important modifiable risk factors assessed during a heart health check are blood pressure, cholesterol, and blood sugar. These three metrics alone significantly influence your long-term cardiovascular outcomes.
At Iluka Medical Centre, we provide onsite pathology, allowing faster testing and quicker follow-up, so your personalized heart health plan can begin without delay.
Now that you know what a heart health check involves, let’s explore why it matters so much, especially in Australia.
Why Heart Disease Prevention Matters: Key Facts & Statistics
Heart disease remains one of the leading causes of death in Australia, but most cardiovascular disease is preventable with early detection and lifestyle management. If you’re wondering whether a heart health check is really necessary, the data makes the answer clear.
According to the Australian Institute of Health and Welfare (AIHW):
- An estimated 3 million Australians aged 18+ (6.7%) were living with heart, stroke, or vascular disease in 2022.
- Around 600,000 adults (3%) reported having coronary heart disease, including angina or a previous heart attack.
- CVD is more common in men (7.6%) than women (5.8%).
And the risk increases significantly with age!
Additional recent national insights show that one Australian experiences a heart attack or stroke every 4 minutes. High blood pressure alone contributes to nearly half of all heart disease cases, yet many people don’t know they have it. Furthermore, more than two-thirds of Australian adults have at least one modifiable risk factor for cardiovascular disease, such as high cholesterol, smoking, obesity, or physical inactivity.
Heart disease develops silently, but the major risk factors are measurable and manageable.
That’s why heart disease prevention and early risk detection through a simple heart check are so powerful. Identifying issues like high blood pressure or elevated cholesterol early can significantly reduce your long-term risk of heart attack or stroke.
7 Silent Risk Factors for Heart Disease You Shouldn’t Ignore

Cardiovascular disease (CVD) rarely happens without warning. It develops over years due to measurable risk factors.
Understanding the key risk factors allows you to take control early. According to the Heart Foundation’s latest statistics, many Australians are living with elevated risk without even realizing it. Let’s break down the key health metrics your GP assesses during a heart health check.
1. High Blood Pressure (Hypertension)
High blood pressure is one of the strongest predictors of heart attack, stroke, and heart failure. It damages blood vessel walls over time and forces the heart to work harder than it should.
Current Australian data shows:
- Men (25%) are more affected than women (22%).
- By age 75, nearly 4 in 5 adults have hypertension.
- Alarmingly, only 5% of adults recognize high blood pressure as a major heart disease risk factor.
Many people in Perth and across WA feel well despite elevated readings, which is why routine blood pressure checks during a heart health check are so important.
2. High Cholesterol
High cholesterol contributes to plaque buildup inside arteries, increasing the risk of coronary heart disease and stroke. Cholesterol is essential for hormone production and cell function, but excess LDL (“bad”) cholesterol can narrow arteries over time.
Key statistics:
- More than 2 in 5 Australian adults (42%) live with high cholesterol.
- Only 7% of Australians recognize high cholesterol as a key risk factor for heart disease.
- It is most common in adults aged 55–64 years.
Because cholesterol has no symptoms, cholesterol testing is a core part of understanding your health metrics during a heart health check.
3. Overweight & Obesity
Excess weight increases the strain on your heart and contributes to high blood pressure, type 2 diabetes, and high cholesterol. In Australia:
- 2 in 3 adults (66%) are overweight or living with obesity.
- Rates are higher in men (71%) than women (61%).
- Around 28% of children and adolescents are above a healthy weight.
Body Mass Index (BMI) is commonly used to estimate weight risk (overweight ≥25, obesity ≥30). However, BMI doesn’t account for muscle mass, age, or body composition, which is why waist circumference and metabolic markers are also assessed during a heart health check.
4. Physical Inactivity
Regular movement improves blood pressure, cholesterol levels, insulin sensitivity, and weight control. However, 75% of Australian adults do not meet recommended physical activity guidelines.
Around 12% report no physical activity at all. Women (73%) are slightly less likely than men to meet guidelines. Only one-third of adults believe low exercise levels significantly increase heart disease risk.
5. Poor Diet
Diet directly affects cholesterol, blood pressure, blood sugar, and weight, all major cardiovascular risk factors.
Australian dietary data shows 93.5% of adults do not meet recommended vegetable intake (5 servings daily). The average adult eats less than half the recommended amount. Unhealthy dietary patterns high in salt, saturated fat, and added sugars continue to contribute to rising heart conditions.
6. Smoking
Smoking damages blood vessels, increases clot formation, and reduces oxygen delivery to the heart. Current figures show around 11% of Australian adults (2.1 million people) are daily smokers, down from 22.4% in 2001.
- Men (12.6%) are more likely than women to smoke daily (8.7%).
- Adults aged 55–64 have the highest smoking rates.
- Only 31% of adults recognize smoking as a key heart disease risk factor.
Even long-term former smokers can carry residual cardiovascular risk, which is why smoking history is assessed during every heart health check.
7. Alcohol Consumption
There is no safe level of alcohol for cardiovascular health.
Excess alcohol contributes to high blood pressure, atrial fibrillation, weight gain, and cardiomyopathy. National data indicates:
- 27% of Australian adults (5.2 million people) exceed alcohol consumption guidelines.
- Men are twice as likely as women to exceed guidelines.
- Only 1 in 10 adults believes alcohol significantly increases heart disease risk.
Reducing alcohol intake is often a simple yet powerful step in heart disease prevention.
Now, let’s discover exactly how to lower your risk and which lifestyle changes truly make a measurable difference.
7 Smart Strategies to Prevent Heart Disease
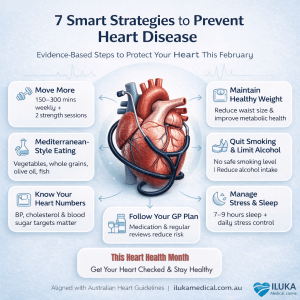
Preventing heart disease is not about extreme changes; it’s about consistent, measurable habits that reduce your cardiovascular risk over time.
1. Move More: Build a Weekly Exercise Routine
Regular physical activity lowers blood pressure, improves cholesterol, supports weight control, and reduces the risk of type 2 diabetes—all major contributors to heart conditions.
According to Australian physical activity guidelines, adults should aim for:
- 150–300 minutes of moderate aerobic activity per week (e.g., brisk walking, cycling, swimming)
OR - 75–150 minutes of vigorous activity (e.g., running, high-intensity training)
PLUS - At least 2 strength-training sessions per week
Even short bursts of movement matter. Five to ten minutes of walking, taking the stairs, gardening, or household activity contributes to heart health.
If you haven’t exercised in a while, start gradually. At Iluka Medical Centre, we often advise patients in Perth’s northern suburbs to begin with simple 20–30 minute walks most days and build from there.
Exercise awareness is one of the most powerful heart health tips—and it’s entirely within your control.
2. Eat for Your Heart: Mediterranean-Style Healthy Diet Tips
Your diet directly affects cholesterol, blood pressure, weight, and blood sugar levels.
Research consistently supports the Mediterranean diet and DASH (Dietary Approaches to Stop Hypertension) eating patterns for cardiovascular disease prevention.
Heart-Healthy Eating Guide:
| Focus On | Limit or Avoid |
| Vegetables (aim for 5+ serves daily) | Processed meats (sausages, bacon, deli meats) |
| Fresh fruits | Highly refined carbohydrates (white bread, pastries, sugary cereals) |
| Whole grains (brown rice, oats, wholemeal bread) | Salt and high-sodium foods (fast food, packaged snacks) |
| Legumes and beans | Sugary drinks (soft drinks, energy drinks, sweetened juices) |
| Nuts and seeds | Saturated fats (fatty red meat, full-fat dairy, coconut oil) |
| Olive oil as your primary cooking fat | Trans fats (fried takeaway foods, commercial baked goods) |
| Fish and seafood (2–3 times per week) | Excess takeaway and highly processed foods |
| Lean poultry | Excess alcohol consumption |
Australian data shows that 93.5% of adults do not meet vegetable intake recommendations, yet increasing vegetable intake alone could reduce cardiovascular risk by an estimated 17%.
Small swaps make a difference:
- Swap white bread for whole grain.
- Swap butter → olive oil
- Swap processed snacks → nuts or fruit
These realistic healthy heart habits significantly reduce long-term risk.
3. Know Your Heart Numbers: Monitor and Act Early
Understanding key health metrics helps you be proactive rather than reactive. Here are the core numbers to know:
Blood Pressure
- Normal: <120/80 mmHg
- High blood pressure significantly increases heart attack and stroke risk.
Home monitoring can be useful, especially if readings fluctuate. Your GP can advise how often to check.
Cholesterol
- Total cholesterol: ideally <5.5 mmol/L
- LDL (“bad” cholesterol): the lower, the better for high-risk individuals
- HDL (“good” cholesterol): protective when higher
Blood Sugar (HbA1c)
- Normal HbA1c: below 5.7%
Elevated blood sugar damages blood vessels and increases CVD risk.
Weight & Waist Circumference
- A BMI 25+ indicates overweight; 30+ indicates obesity
- Waist measurement risk thresholds:
- Men: >102 cm
- Women: >88 cm
Even a modest 3–5% weight reduction improves blood pressure, cholesterol, and glucose levels. Regular monitoring through a heart health check ensures you stay on track.
4. Maintain a Healthy Weight (Without Extreme Dieting)
Excess abdominal fat increases inflammatory markers and insulin resistance. And both are linked to cardiovascular disease. Weight management doesn’t require crash dieting. Sustainable changes work best:
- Increase daily movement
- Improve portion control
- Prioritise fibre-rich foods
- Reduce late-night snacking
- Seek professional guidance if needed
At Iluka Medical Centre, we often combine GP care with dietary support to build a personalized heart health plan tailored to each patient’s risk profile.
5. Quit Smoking & Limit Alcohol Intake
Smoking
Smoking damages blood vessels, accelerates plaque buildup, and increases clot formation.
Although smoking rates have declined in Australia, it remains a major preventable contributor to heart disease. Quitting reduces cardiovascular risk rapidly—within one year, heart attack risk significantly decreases.
If you smoke, speak with your GP about nicotine replacement therapy or prescription support.
Alcohol
There is no safe level of alcohol for cardiovascular protection. Excess alcohol contributes to high blood pressure, atrial fibrillation, and weight gain. Reducing alcohol intake can meaningfully improve blood pressure and overall heart health.
6. Manage Stress, Sleep & Mental Health
Chronic stress increases cortisol levels, raises blood pressure, and encourages unhealthy coping behaviors such as overeating or smoking.
Healthy stress management strategies include:
- Regular exercise
- Mindfulness or meditation
- Deep breathing exercises
- Adequate sleep (7–9 hours per night)
- Seeking support for anxiety or depression
Mental health and cardiovascular health are closely linked. Addressing both is a core part of comprehensive heart health care.
7. Take Medications as Prescribed & Attend Follow-Ups
For some patients, lifestyle changes alone are not enough. If your heart health check identifies moderate to high cardiovascular risk, your GP may recommend medication such as:
- Blood pressure medication
- Cholesterol-lowering therapy (statins)
- Blood sugar control medication
Medication adherence significantly reduces heart attack and stroke risk when clinically indicated. Regular follow-up appointments allow adjustment of treatment plans and monitoring of progress.
Conclusion: One Simple Check Could Save Your Life
Heart disease prevention is possible, and it begins with knowing your numbers. A simple heart health check brings together blood pressure checks, cholesterol testing, and blood sugar measurement so you can see your personal risk and take action with a clear, personalized heart health plan.
This Heart Health Month, don’t wait for symptoms to appear. Be proactive. It’s the single best gift you can give yourself and your family. Let us help you understand your results and turn them into a clear, practical plan that supports lasting heart health.
Worried you might have a hidden heart risk and don’t know where to start?
Get Your Heart Checked Before It’s Too Late
At Iluka Medical Centre, we combine GP expertise with onsite pathology and allied health support to move you from risk to results quickly and practically.
We’ll explain what your numbers mean, create a tailored heart health plan (diet, exercise, and medication if needed), and arrange fast onsite pathology so you don’t wait for answers.
Be proactive—early detection is the most effective strategy for preventing heart disease.
Book Your Heart Health Check Now
FAQs
When is Heart Month in Australia?
February is Heart Health Month in Australia. It’s a timely reminder to check your heart health and take proactive steps toward cardiovascular disease prevention.
Who should get a heart health check, and how often?
Adults aged 45 and over should consider regular checks. People with diabetes, a strong family history, high blood pressure, high cholesterol, smokers, or Aboriginal and Torres Strait Islander people should start earlier (often from age 30–35). Frequency depends on heart disease risk. Low-risk adults may be reviewed every 1–3 years, while higher-risk patients need more frequent follow-up as advised by their GP.
What tests are included in a heart health check?
Common tests include blood pressure checks, a blood test for cholesterol and blood sugar (often fasting or HbA1c), BMI/waist measurement, and stroke/heart-risk scoring. Additional tests (ECG, cardiac imaging) are ordered if clinically indicated.
Can a heart health check prevent a heart attack?
A heart health check can’t guarantee prevention, but it identifies modifiable risk factors early. Treating high blood pressure, lowering cholesterol, improving blood sugar and adopting healthy habits markedly reduce the likelihood of heart attack and stroke.
What BP level is considered a medical emergency (stroke risk)?
A hypertensive crisis (a medical emergency) is typically defined as a reading above 180/120 mmHg. If this occurs, especially with chest pain, severe headache, vision changes, breathlessness, or weakness, seek immediate health care.
Is the heart health check painful?
No, most of the check is non-invasive (questions, blood pressure cuff, measurements). Blood tests involve a quick needle for a small blood sample; most people describe mild, brief discomfort only.
How do I prepare for a heart health check?
Bring a list of current medications, any family history of heart disease, and typical lifestyle details (diet, activity, smoking). Your GP will advise if fasting is needed for cholesterol testing.
Data Sources & References:
The statistics and evidence presented in the blog are drawn from reputable Australian health authorities to ensure accuracy and reliability. Primary sources include:
